Search
- Page Path
- HOME > Search
- Clinical Study
- Fasting and Postprandial Hyperglycemia: Their Predictors and Contributions to Overall Hyperglycemia in Korean Patients with Type 2 Diabetes
- Jaecheol Moon, Ji Young Kim, Soyeon Yoo, Gwanpyo Koh
- Endocrinol Metab. 2020;35(2):290-297. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.290
- 6,881 View
- 201 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
This study aimed to identify factors that affect fasting hyperglycemia (FHG) and postprandial hyperglycemia (PPG) and their contributions to overall hyperglycemia in Korean patients with type 2 diabetes mellitus (T2DM).
Methods
This was a retrospective study conducted on 194 Korean T2DM patients with 7-point self-monitoring blood glucose (SMBG) profiles plotted in 4 days in 3 consecutive months. We calculated the areas corresponding to FHG and PPG (area under the curve [AUC]FHG and AUCPPG) and contributions (%) in the graph of the 7-point SMBG data. The levels of glycated hemoglobin (HbA1c) were categorized by tertiles, and the contributions of FHG and PPG were compared.
Results
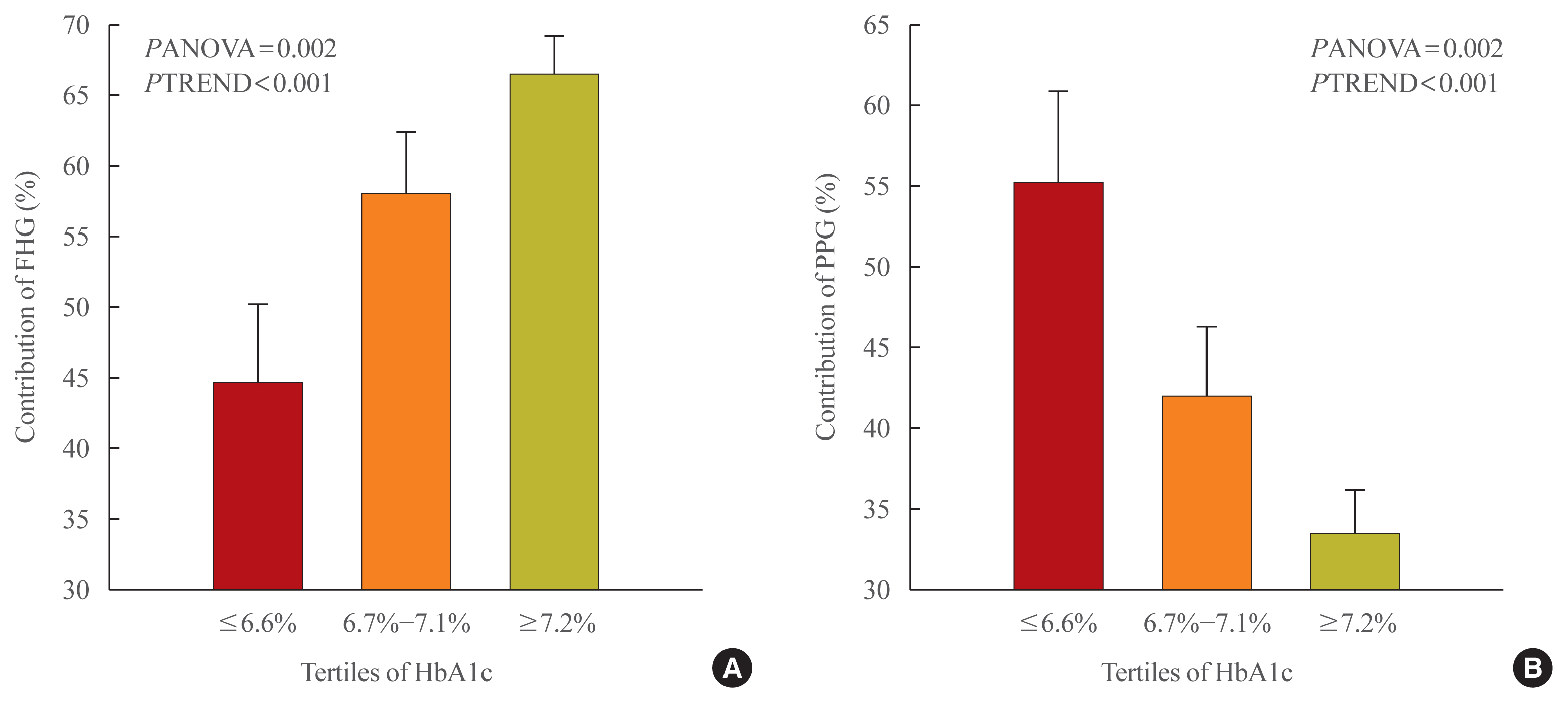
The relative contribution of FHG increased (44.7%±5.6%, 58.0%±4.4%, 66.5%±2.8%; PANOVA=0.002, PTREND <0.001), while that of PPG decreased (55.3%±5.5%, 42.0%±4.4%, 33.5%±2.8%; PANOVA=0.002, PTREND <0.001) with the elevated HbA1c. Multivariate analysis showed that HbA1c (β=0.615, P<0.001), waist circumference (β=0.216, P=0.042), and triglyceride (β=0.121, P=0.048) had a significant association with AUCFHG. Only HbA1c (β=0.231, P=0.002) and age (β=0.196, P=0.009) was significantly associated with AUCPPG.
Conclusion
The data suggested that in Korean T2DM patients, FHG predominantly contributed to overall hyperglycemia at higher HbA1c levels, whereas it contributed to PPG at lower HbA1c levels. It is recommended that certain factors, namely age, degree of glycemic control, obesity, or triglyceride levels, should be considered when prescribing medications for T2DM patients. -
Citations
Citations to this article as recorded by- Prospective study of the association between chronotype and cardiometabolic risk among Chinese young adults
Tingting Li, Yang Xie, Shuman Tao, Liwei Zou, Yajuan Yang, Fangbiao Tao, Xiaoyan Wu
BMC Public Health.2023;[Epub] CrossRef - Effects of mulberry twig alkaloids(Sangzhi alkaloids) and metformin on blood glucose fluctuations in combination with premixed insulin-treated patients with type 2 diabetes
Ziyu Meng, Chengye Xu, Haoling Liu, Xinyuan Gao, Xinyu Li, Wenjian Lin, Xuefei Ma, Changwei Yang, Ming Hao, Kangqi Zhao, Yuxin Hu, Yi Wang, Hongyu Kuang
Frontiers in Endocrinology.2023;[Epub] CrossRef - Evaluating Triglyceride and Glucose Index as a Simple and Easy-to-Calculate Marker for All-Cause and Cardiovascular Mortality
Kyung-Soo Kim, Sangmo Hong, You-Cheol Hwang, Hong-Yup Ahn, Cheol-Young Park
Journal of General Internal Medicine.2022; 37(16): 4153. CrossRef - A new approach for investigating the relative contribution of basal glucose and postprandial glucose to HbA1C
Jing Ma, Hua He, Xiaojie Yang, Dawei Chen, Cuixia Tan, Li Zhong, Qiling Du, Xiaohua Wu, Yunyi Gao, Guanjian Liu, Chun Wang, Xingwu Ran
Nutrition & Diabetes.2021;[Epub] CrossRef - The Clinical Characteristics of Gestational Diabetes Mellitus in Korea: A National Health Information Database Study
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
Endocrinology and Metabolism.2021; 36(3): 628. CrossRef
- Prospective study of the association between chronotype and cardiometabolic risk among Chinese young adults

- Clinical Study
- Correlation of Glypican-4 Level with Basal Active Glucagon-Like Peptide 1 Level in Patients with Type 2 Diabetes Mellitus
- Sang Ah Lee, Gwanpyo Koh, Suk Ju Cho, So-Yeon Yoo, Sang Ouk Chin
- Endocrinol Metab. 2016;31(3):439-445. Published online September 26, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.3.439
- 4,040 View
- 41 Download
- 8 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background Previous studies have reported that glypican-4 (GPC4) regulates insulin signaling by interacting with insulin receptor and through adipocyte differentiation. However, GPC4 has not been studied with regard to its effects on clinical factors in patients with type 2 diabetes mellitus (T2DM). We aimed to identify factors associated with GPC4 level in T2DM.
Methods Between January 2010 and December 2013, we selected 152 subjects with T2DM and collected serum and plasma into tubes pretreated with aprotinin and dipeptidyl peptidase-4 inhibitor to preserve active gastric inhibitory polypeptide (GIP) and glucagon-like peptide 1 (GLP-1). GPC4, active GLP-1, active GIP, and other factors were measured in these plasma samples. We performed a linear regression analysis to identify factors associated with GPC4 level.
Results The subjects had a mean age of 58.1 years, were mildly obese (mean body mass index [BMI], 26.1 kg/m2), had T2DM of long-duration (mean, 101.3 months), glycated hemoglobin 7.5%, low insulin secretion, and low insulin resistance (mean homeostatic model assessment of insulin resistance [HOMA-IR], 1.2). Their mean GPC4 was 2.0±0.2 ng/mL. In multivariate analysis, GPC4 was independently associated with age (β=0.224,
P =0.009), and levels of active GLP-1 (β=0.171,P =0.049) and aspartate aminotransferase (AST; β=–0.176,P =0.043) after being adjusted for other clinical factors.Conclusion GPC4 was independently associated with age, active GLP-1, and AST in T2DM patients, but was not associated with HOMA-IR and BMI, which are well known factors related to GPC4. Further study is needed to identify the mechanisms of the association between GPC4 and basal active GLP-1 levels.
-
Citations
Citations to this article as recorded by- How Reliable are Commercially Available Glypican4 ELISA
Kits?
Joseph P. Buhl, Antje Garten, Jürgen Kratzsch, Wieland Kiess, Melanie Penke
Experimental and Clinical Endocrinology & Diabetes.2022; 130(02): 110. CrossRef - Serum glypican-4 is associated with the 10-year clinical outcome of patients with peripheral artery disease
Axel Muendlein, Christine Heinzle, Andreas Leiherer, Kathrin Geiger, Eva Maria Brandtner, Stella Gaenger, Peter Fraunberger, Christoph H. Saely, Heinz Drexel
International Journal of Cardiology.2022; 369: 54. CrossRef - Berberine activates the β-catenin/TCF4 signaling pathway by down-regulating miR-106b to promote GLP-1 production by intestinal L cells
Jiao Wang, Li-Rui Wei, Yan-Ling Liu, Cheng-Zhi Ding, Feng Guo, Jiao Wang, Qian Qin, Feng-Jiao Huang, Ying Xin, Sheng-Nan Ma, Qiu-Ran Zhai, Shou-Jun Wang, Gui-Jun Qin
European Journal of Pharmacology.2021; 911: 174482. CrossRef - Increased Glypican-4 Levels Are Associated with Obesity in Adolescents
Huseyin Dag, Nevin Cetin Dag, Okan Dikker
Iranian Journal of Pediatrics.2019;[Epub] CrossRef - Serum glypican 4 level in obese children and its relation to degree of obesity
Chutima Leelalertlauw, Manassawee Korwutthikulrangsri, Pat Mahachoklertwattana, Suwannee Chanprasertyothin, Patcharin Khlairit, Sarunyu Pongratanakul, Preamrudee Poomthavorn
Clinical Endocrinology.2017; 87(6): 689. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Efficacy and Safety of Single‐ or Double‐Drug Antidiabetic Regimens in the Treatment of Type 2 Diabetes Mellitus: A Network Meta‐Analysis
Xi‐Ling Yang, Mi‐Ma Duo‐Ji, Zi‐Wen Long
Journal of Cellular Biochemistry.2017; 118(12): 4536. CrossRef
- How Reliable are Commercially Available Glypican4 ELISA
Kits?

- Obesity and Metabolism
- Factors Associated with Glycemic Variability in Patients with Type 2 Diabetes: Focus on Oral Hypoglycemic Agents and Cardiovascular Risk Factors
- Soyeon Yoo, Sang-Ouk Chin, Sang-Ah Lee, Gwanpyo Koh
- Endocrinol Metab. 2015;30(3):352-360. Published online August 4, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.3.352
- 3,878 View
- 46 Download
- 9 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background The role of glycemic variability (GV) in development of cardiovascular diseases remains controversial, and factors that determine glucose fluctuation in patients with diabetes are unknown. We investigated relationships between GV indices, kinds of oral hypoglycemic agents (OHAs), and cardiovascular risk factors in patients with type 2 diabetes mellitus (T2DM).
Methods We analyzed 209 patients with T2DM. The GV index (standard deviation [SD] and mean absolute glucose change [MAG]) were calculated from 7-point self-monitoring of blood glucose profiles. The patients were classified into four groups according to whether they take OHAs known as GV-lowering (A) and GV-increasing (B): 1 (A only), 2 (neither), 3 (both A and B), and 4 (B only). The 10-year risk for atherosclerotic cardiovascular disease (ASCVD) was calculated using the Pooled Cohort Equations.
Results GV indices were significantly higher in patients taking sulfonylureas (SUs), but lower in those taking dipeptidyl peptidase-4 inhibitors. In hierarchical regression analysis, the use of SUs remained independent correlates of the SD (β=0.209,
P =0.009) and MAG (β=0.214,P =0.011). In four OHA groups, GV indices increased progressively from group 1 to group 4. However, these did not differ according to quartiles of 10-year ASCVD risk.Conclusion GV indices correlated significantly with the use of OHAs, particularly SU, and differed significantly according to combination of OHAs. However, cardiovascular risk factors and 10-year ASCVD risk were not related to GV indices. These findings suggest that GV is largely determined by properties of OHAs and not to cardiovascular complications in patients with T2DM.
-
Citations
Citations to this article as recorded by- Prognostic value of longitudinal HbA1c variability in predicting the development of diabetic sensorimotor polyneuropathy among patients with type 2 diabetes mellitus: A prospective cohort observational study
Yun‐Ru Lai, Wen‐Chan Chiu, Chih‐Cheng Huang, Ben‐Chung Cheng, I‐Hsun Yu, Chia‐Te Kung, Ting Yin Lin, Hui Ching Chiang, Chun‐En Aurea Kuo, Cheng‐Hsien Lu
Journal of Diabetes Investigation.2024; 15(3): 326. CrossRef - Influence of dipeptidyl peptidase-4 inhibitors on glycemic variability in patients with type 2 diabetes: A meta-analysis of randomized controlled trials
Shangyu Chai, Ruya Zhang, Ye Zhang, Richard David Carr, Yiman Zheng, Swapnil Rajpathak, Miao Yu
Frontiers in Endocrinology.2022;[Epub] CrossRef - Glycemic Variability in Subjects with Diabetes and Hypogonadism during Testosterone Replacement Treatment: A Pilot Study
Giuseppe Defeudis, Ernesto Maddaloni, Giovanni Rossini, Alfonso Maria Di Tommaso, Rossella Mazzilli, Paolo Di Palma, Paolo Pozzilli, Nicola Napoli
Journal of Clinical Medicine.2022; 11(18): 5333. CrossRef - New Insights into the Role of Visit-to-Visit Glycemic Variability and Blood Pressure Variability in Cardiovascular Disease Risk
Jin J. Zhou, Daniel S. Nuyujukian, Peter D. Reaven
Current Cardiology Reports.2021;[Epub] CrossRef - Prevalence of glycemic variability and factors associated with the glycemic arrays among end-stage kidney disease patients on chronic hemodialysis
Abdul Hanif Khan Yusof Khan, Nor Fadhlina Zakaria, Muhammad Adil Zainal Abidin, Nor Azmi Kamaruddin
Medicine.2021; 100(30): e26729. CrossRef - Dipeptidyl-Peptidase-IV Inhibitors, Imigliptin and Alogliptin, Improve Beta-Cell Function in Type 2 Diabetes
Xu Liu, Yang Liu, Hongzhong Liu, Haiyan Li, Jianhong Yang, Pei Hu, Xinhua Xiao, Dongyang Liu
Frontiers in Endocrinology.2021;[Epub] CrossRef - HbA 1C variability and hypoglycemia hospitalization in adults with type 1 and type 2 diabetes: A nested case-control study
Victor W. Zhong, Juhaeri Juhaeri, Stephen R. Cole, Christina M. Shay, Penny Gordon-Larsen, Evangelos Kontopantelis, Elizabeth J. Mayer-Davis
Journal of Diabetes and its Complications.2018; 32(2): 203. CrossRef - Glucose fluctuation and the resultant endothelial injury are correlated with pancreatic β cell dysfunction in patients with coronary artery disease
Makoto Murata, Hitoshi Adachi, Shigeru Oshima, Masahiko Kurabayashi
Diabetes Research and Clinical Practice.2017; 131: 107. CrossRef - Efficacy of lifestyle interventions in patients with type 2 diabetes: A systematic review and meta-analysis
Xiao-Li Huang, Jian-Hua Pan, Dan Chen, Jing Chen, Fang Chen, Tao-Tao Hu
European Journal of Internal Medicine.2016; 27: 37. CrossRef
- Prognostic value of longitudinal HbA1c variability in predicting the development of diabetic sensorimotor polyneuropathy among patients with type 2 diabetes mellitus: A prospective cohort observational study

- Obesity and Metabolism
- Apolipoprotein B Is Related to Metabolic Syndrome Independently of Low Density Lipoprotein Cholesterol in Patients with Type 2 Diabetes
- Younghyup Lim, Soyeon Yoo, Sang Ah Lee, Sang Ouk Chin, Dahee Heo, Jae Cheol Moon, Shinhang Moon, Kiyoung Boo, Seong Taeg Kim, Hye Mi Seo, Hyeyoung Jwa, Gwanpyo Koh
- Endocrinol Metab. 2015;30(2):208-215. Published online June 30, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.2.208
- 4,540 View
- 46 Download
- 19 Web of Science
- 21 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Increased low density lipoprotein cholesterol (LDL-C) level and the presence of metabolic syndrome (MetS) are important risk factors for cardiovascular disease (CVD) in type 2 diabetes mellitus (T2DM). Recent studies demonstrated apolipoprotein B (apoB), a protein mainly located in LDL-C, was an independent predictor of the development of CVD especially in patients with T2DM. The aim of this study was to investigate the relationship between apoB and MetS in T2DM patients.
Methods We analyzed 912 patients with T2DM. Fasting blood samples were taken for glycated hemoglobin, high-sensitivity C-reactive protein, total cholesterol, triglyceride (TG), high density lipoprotein cholesterol, LDL-C, and apoB. MetS was defined by the modified National Cholesterol Education Program Adult Treatment Panel III criteria. We performed a hierarchical regression analysis with apoB as the dependent variable. Age, sex, the number of components of MetS and LDL-C were entered at model 1, the use of lipid-lowering medications at model 2, and the individual components of MetS were added at model 3.
Results Seventy percent of total subjects had MetS. ApoB level was higher in subjects with than those without MetS (104.5±53.3 mg/dL vs. 87.7±33.7 mg/dL,
P <0.01) even after adjusting for LDL-C. ApoB and LDL-C were positively correlated to the number of MetS components. The hierarchical regression analysis showed that the increasing number of MetS components was associated with higher level of apoB at step 1 and step 2 (β=0.120,P <0.001 and β=0.110,P <0.001, respectively). At step 3, TG (β=0.116,P <0.001) and systolic blood pressure (β=0.099,P <0.05) were found to significantly contribute to apoB.Conclusion In patients with T2DM, apoB is significantly related to MetS independently of LDL-C level. Of the components of MetS, TG, and systolic blood pressure appeared to be determinants of apoB.
-
Citations
Citations to this article as recorded by- ApoB100 and Atherosclerosis: What’s New in the 21st Century?
Dimitris Kounatidis, Natalia G. Vallianou, Aikaterini Poulaki, Angelos Evangelopoulos, Fotis Panagopoulos, Theodora Stratigou, Eleni Geladari, Irene Karampela, Maria Dalamaga
Metabolites.2024; 14(2): 123. CrossRef - Association of apolipoproteins and lipoprotein(a) with metabolic syndrome: a systematic review and meta-analysis
Juan R. Ulloque-Badaracco, Ali Al-kassab-Córdova, Enrique A. Hernandez-Bustamante, Esteban A. Alarcon-Braga, Miguel Huayta-Cortez, Ximena L. Carballo-Tello, Rosa A. Seminario-Amez, Percy Herrera-Añazco, Vicente A. Benites-Zapata
Lipids in Health and Disease.2023;[Epub] CrossRef - Current Data and New Insights into the Genetic Factors of Atherogenic Dyslipidemia Associated with Metabolic Syndrome
Lăcramioara Ionela Butnariu, Eusebiu Vlad Gorduza, Elena Țarcă, Monica-Cristina Pânzaru, Setalia Popa, Simona Stoleriu, Vasile Valeriu Lupu, Ancuta Lupu, Elena Cojocaru, Laura Mihaela Trandafir, Ștefana Maria Moisă, Andreea Florea, Laura Stătescu, Minerva
Diagnostics.2023; 13(14): 2348. CrossRef - Apolipoprotein B compared with low-density lipoprotein cholesterol in the atherosclerotic cardiovascular diseases risk assessment
Federica Galimberti, Manuela Casula, Elena Olmastroni
Pharmacological Research.2023; 195: 106873. CrossRef - Circulating lipids and breast cancer prognosis in the Malmö diet and cancer study
Sixten Harborg, Thomas P. Ahern, Maria Feldt, Ann H. Rosendahl, Deirdre Cronin-Fenton, Olle Melander, Signe Borgquist
Breast Cancer Research and Treatment.2022; 191(3): 611. CrossRef - Metabolic disorders in patients with impaired glucose tolerance, with or without underlying ischaemic heart disease
Milena Brkić, Danijel Đekić, Jelena Jovanić, Goran Topić, Aleksandra Grbić, Tatjana Šutilović
Scripta Medica.2022; 53(3): 175. CrossRef - Genetics of Cholesterol-Related Genes in Metabolic Syndrome: A Review of Current Evidence
Sok Kuan Wong, Fitri Fareez Ramli, Adli Ali, Nurul ‘Izzah Ibrahim
Biomedicines.2022; 10(12): 3239. CrossRef - Prevalence of ApoB100 rs693 gene polymorphism in metabolic syndrome among female students at King Abdulaziz University
Rana A. Alghamdi, Maryam H. Al-Zahrani, Maha J. Balgoon, Nuha A. Alkhattabi
Saudi Journal of Biological Sciences.2021; 28(6): 3249. CrossRef - Local ablation of gastric cancer by reconstituted apolipoprotein B lipoparticles carrying epigenetic drugs
Chia-Lung Yang, Ying-Jui Chao, Hao-Chen Wang, Ya-Chin Hou, Caleb Gonshen Chen, Chia-Ching Chang, Yan-Shen Shan
Nanomedicine: Nanotechnology, Biology and Medicine.2021; 37: 102450. CrossRef - Cardiovascular Biomarkers of Obesity and Overlap With Cardiometabolic Dysfunction
Emily S. Lau, Samantha M. Paniagua, Shahrooz Zarbafian, Udo Hoffman, Michelle T. Long, Shih‐Jen Hwang, Paul Courchesne, Chen Yao, Jiantao Ma, Martin G. Larson, Daniel Levy, Ravi V. Shah, Jennifer E. Ho
Journal of the American Heart Association.2021;[Epub] CrossRef - The association of ecg TV1>TV6 phenomenon as electrophysiological sign of metabolic myocardial disorders with risk factors for ischemic heart disease in the population of 25–44 years
N. A. Kuzminykh, L. V. Shcherbakova, V. S. Shramko, D. V. Denisova, Yu. I. Ragino
Ateroscleroz.2021; 17(2): 22. CrossRef - Regulation of Apolipoprotein B by Natural Products and Nutraceuticals: A Comprehensive Review
Mohammad Bagherniya, Thomas P. Johnston, Amirhossein Sahebkar
Current Medicinal Chemistry.2021; 28(7): 1363. CrossRef - Apolipoprotein B and non-high-density lipoprotein cholesterol reveal a high atherogenicity in individuals with type 2 diabetes and controlled low-density lipoprotein-cholesterol
Liliana Fonseca, Sílvia Paredes, Helena Ramos, José Carlos Oliveira, Isabel Palma
Lipids in Health and Disease.2020;[Epub] CrossRef - Menopause-Associated Lipid Metabolic Disorders and Foods Beneficial for Postmenopausal Women
Seong-Hee Ko, Hyun-Sook Kim
Nutrients.2020; 12(1): 202. CrossRef - Lipoprotein A, combined with alanine aminotransferase and aspartate aminotransferase, contributes to predicting the occurrence of NASH: a cross-sectional study
Yu Zhang, He He, Yu-Ping Zeng, Li-Dan Yang, Dan Jia, Zhen-Mei An, Wei-Guo Jia
Lipids in Health and Disease.2020;[Epub] CrossRef - Novel and traditional lipid profiles in Metabolic Syndrome reveal a high atherogenicity
Sílvia Paredes, Liliana Fonseca, Laura Ribeiro, Helena Ramos, José Carlos Oliveira, Isabel Palma
Scientific Reports.2019;[Epub] CrossRef - Serum apolipoprotein B is associated with increased risk of metabolic syndrome among middle‐aged and elderly Chinese: A cross‐sectional and prospective cohort study
Rui Du, Xueyan Wu, Kui Peng, Lin Lin, Mian Li, Yu Xu, Min Xu, Yuhong Chen, Donghui Li, Jieli Lu, Yufang Bi, Weiqing Wang, Guang Ning
Journal of Diabetes.2019; 11(9): 752. CrossRef - The role of metabolism disorders, inflammation, myocardial injury in development chronic heart failure in metabolic syndrome patients
A. P. Roytman, T. A. Fedorova, E. A. Ivanova, A. V. Bugrov, V. V. Dolgov
Laboratornaya sluzhba.2018; 7(4): 5. CrossRef - Serum apoB levels independently predict the development of non‐alcoholic fatty liver disease: A 7‐year prospective study
Jinghua Wang, Wanlin Zhu, Shujun Huang, Lei Xu, Min Miao, Chenjiao Wu, Chaohui Yu, Youming Li, Chengfu Xu
Liver International.2017; 37(8): 1202. CrossRef - Comprehensive assessment of lipoprotein subfraction profiles according to glucose metabolism status, and association with insulin resistance in subjects with early-stage impaired glucose metabolism
Jie-Eun Lee, Se Hee Min, Dong-Hwa Lee, Tae Jung Oh, Kyoung Min Kim, Jae Hoon Moon, Sung Hee Choi, Kyong Soo Park, Hak Chul Jang, Soo Lim
International Journal of Cardiology.2016; 225: 327. CrossRef - Association of Serum Apolipoprotein B with the Increased Risk of Diabetes in Korean Men
Hyo Hee Lim, Oh Yoen Kim
Clinical Nutrition Research.2016; 5(3): 204. CrossRef
- ApoB100 and Atherosclerosis: What’s New in the 21st Century?

- A Case of Kallmann's Syndrome with Frontal Lobe Atrophy and Mental Retardation.
- Soyoung Hyun, Seungguk Park, Dong Gu Kang, Seung Uk Jeong, Dea Ho Lee, Gwanpyo Koh
- Endocrinol Metab. 2010;25(2):142-146. Published online June 1, 2010
- DOI: https://doi.org/10.3803/EnM.2010.25.2.142
- 1,712 View
- 27 Download
-
 Abstract
Abstract
 PDF
PDF - Kallmann's syndrome is a rare condition, and this is defined as hypogonadotropic hypogonadism and anosmia or hyposmia. The syndrome may be associated with cleft lip, cleft palate, color blindness, skeletal abnormalities, renal agenesis, sensory neural hearing loss, obesity, etc. About 10 cases of Kallmann's syndrome have been reported in Korea, but there are no reports on cases of Kallmann's syndrome with atrophy of the frontal lobe, severe mental retardation and unilateral renal agenesis. We experienced a case of 17-year-old boy with abnormalities of the olfactory system, as was noted on magnetic resonance imaging (MRI). He had an atrophy of the frontal lobe, mental retardation, a micropenis and unilateral renal agenesis. Hormonal assay documented low levels of luteinizing hormone (LH), follicle stimulating hormone (FSH), testosterone and thyroid-stimulating hormone (TSH). So, we report here on an unusual case of Kallmann's syndrome along with briefly reviewing the relevant medical literature.

- Clinical Usefulness of Glucose Testing from the Forearm in Diabetic Patients.
- Sang Wook Lee, Suk Chon, Seungjoon Oh, Jeong taek Woo, Sung Woon Kim, Jin Woo Kim, Young Seol Kim, Jeong Ryung Paeng, Gwanpyo Koh, Hak Hyun Nam
- J Korean Endocr Soc. 2006;21(4):281-289. Published online August 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.4.281
- 1,773 View
- 21 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Self monitoring of blood glucose plays an important role in the management of diabetes. However, traditional finger prick testing causes pain and so compliance with self monitoring of blood glucose is usually poor. Using an alternative site for sampling may reduce the level of pain and be beneficial for improving the compliance of diabetic patients. We evaluated the accuracy and acceptability of blood glucose testing from the forearm by analyzing the performance of the CareSens(R) (i-Sens, Inc. Korea) device for diabetic patients. METHODS: We measured the glucose level at the forearm by use of CareLance(R) (vaccum assisted lancing device) and also at the finger tip simultaneously by use of the CareSens(R) device at fasting and postprandial 2 hours, respectively. At the same time, the glucose levels of venous samples were checked by the laboratory method (BIOSEN 5030, EKF, Germany) and compared with those glucose level measured by the CareSens(R) device. We also checked the ease of use of the CareLance(R) and the associated pain of the patients by means of a visual analogue scale (VAS) at the time of blood sampling. RESULTS: The glucose level obtained from the forearm and finger tip correlated well with that from the laboratory method, respectively. Error grid analysis showed that 100% of the measurements were clinically acceptable; forearm blood glucose testing by use of CareLance(R) was less painful and it was as easy to use as the finger prick (P < 0.05 and P = 0.04, respectively). CONCLUSION: Forearm testing is an acceptable alternative to finger prick testing for measuring blood glucose in diabetic patients. -
Citations
Citations to this article as recorded by- Accuracy Evaluation of the Alternative Site Blood Glucose Test Using Error Grid
Kyung-Soon Park, Eun-Jong Cha
Journal of Biomedical Engineering Research.2011; 32(1): 25. CrossRef
- Accuracy Evaluation of the Alternative Site Blood Glucose Test Using Error Grid

- A Case Of Transient Hyporeninemic Hypoaldosteronism After Unilateral Adrenalrectomy for Aldosterone-Producing Adenoma.
- Jungho Suh, Gwanpyo Koh, Keun Yong Park, Jongwook Hong, Suk Chon, Seungjoon Oh, Jeong taek Woo, Sung Woon Kim, Jin Woo Kim, Young Seol Kim
- J Korean Endocr Soc. 2005;20(5):502-506. Published online October 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.5.502
- 2,048 View
- 31 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Primary aldosteronism is due to either a unilateral adrenal adenoma or bilateral hyperplasia of the adrenal cortex in most cases. A unilateral adrenalectomy in hypertensive and hypokalemic patients, with a well-documented adrenal adenoma, is usually followed by the correction of hypokalemia in all subjects, with the cure of hypertension in 60 to 87% of patients. Here, a unique case, in which a unilateral adrenalectomy for the removal of an adrenal adenoma was followed by severe hyperkalemia, low levels of plasma renin activity and serum aldosterone, suggestive of chronic suppression of the renin-aldosterone axis, is reported. In a follow-up Lasix stimulation test on the 70th day after surgery, the suppression of the renin-aldosterone axis was resolved, indicating the suppression was transient. Patients undergoing a unilateral adrenalectomy for an aldosterone-producing adenoma should be closely followed up to avoid severe hyperkalemia.
-
Citations
Citations to this article as recorded by- A Case of Persistent Hyperkalemia After Unilateral Adrenalectomy for Aldosterone-Producing Adenoma
Min Jae Yang, Seung Jin Han, Min Seok Lee, Eun Kyung Kim, Hae Jin Kim, Dae Jung Kim, Yoon Sok Chung, Tae Hee Lee, Jang Hee Kim, Kwan Woo Lee
Journal of Korean Endocrine Society.2009; 24(3): 201. CrossRef
- A Case of Persistent Hyperkalemia After Unilateral Adrenalectomy for Aldosterone-Producing Adenoma

- A Case of Thyroid Abscess Associated with Lymphocytic Thyroidits.
- Hyoun Jung Chin, Mi Kwang Kwon, Yeehuung Kim, Gwanpyo Koh, Keun Yong Park, Suk Chon, Seungjoon Oh, Jeong Taek Woo, Sung Woon Kim, Jin Woo Kim, Young Seol Kim, Moon Ho Yang
- J Korean Endocr Soc. 2005;20(4):385-389. Published online August 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.4.385
- 1,596 View
- 17 Download

- Mutational Analysis of Gsalpha Protein in Fibrous dysplasia of the Bone.
- Sang Youl Rhee, Jeong Taek Woo, Gwanpyo Koh, Seungjoon Oh, Sung Woon Kim, Jin Woo Kim, Young Seol Kim, Yong Koo Park
- J Korean Endocr Soc. 2005;20(2):142-147. Published online April 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.2.142
- 1,482 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Fibrous dysplasia of the bone(FD) is a benign fibrous bone lesion which usually involves the long bones of the extremities. FD may be asymptomatic, but often leads to bone deformity and pathological fracture. The disease is caused by a somatic mutation in the Gsalpha protein, which is responsible for intracellular signal transduction. METHODS: Mutations in the GNAS1 gene, which codes for Gsalpha protein, was investigated in 34 patients with monostotic and polyostotic FD and McCune-Albright syndrome. DNA was extracted from formalin-fixed, paraffin embedded bone tissues, and exons 8 and 9 of the GNAS1 gene amplified using a polymerase chain reaction(PCR). Subsequently, plasmid cloning and DNA sequencing analysis were performed. RESULTS: The PCR was successfully performed in 5 patients with monostotic FD. However, the sequencing analysis failed to identify any significant point mutations in exons 8 or 9 of GNAS1. Nevertheless, 3 point mutations were observed in the intron of the GNAS1 gene in 2 samples. CONCLUSION: In addition to the previously known somatic mutations of the GNAS1 gene, this study suggests that fibrous dysplasia of the bone might be associated with another point mutations of the GNAS1 gene


 KES
KES

 First
First Prev
Prev



